Comments due by Feb. 14, 2016
It was a gray, damp January afternoon a few years back when I visited the
Jiangfeng wholesale poultry market on the outskirts of Guangzhou, in the
southern Chinese province of Guangdong. With its bleak wire enclosures and
grid of cement paths, the place had the feel of a neglected 1970s era urban zoo.
And despite the comparatively narrow range of species there — chickens,
geese, ducks, quails and partridges, mostly, with a smattering of rabbits and
one large slumbering hog — it smelled like one, too. As I walked around,
watched suspiciously by the market’s handsome young security guards, a slimy
mix of bird droppings and decomposing feathers slowly crept up the heels of
my clogs.
Every few months, it seems, an invasive virus from a distant land attacks
the Americas: dengue, chikungunya and, most recently, Zika. But the
pathogens that frighten me most are novel strains of avian influenza.
I’d come to see their birthplace. Highly virulent and easily transmissible,
these viruses emerge from openair poultry farms and markets of the kind that stretch across Asia. Thanks to rising demand for chicken and other poultry,
they’ve been surfacing at an accelerated clip, causing nearly 150 percent more
outbreaks in 2015 than in 2014. And in late 2014, one strain managed to cross
the ocean that had previously prevented its spread into the Americas,
significantly expanding its reach across the globe.
Novel avian influenza viruses are mongrels, born when the influenza
viruses that live harmlessly inside the bodies of wild ducks, geese and other
waterfowl mix with those of domesticated animals like the ones at Jiangfeng,
especially poultry but also pigs. It’s possible to squelch their emergence. One
way is to protect domesticated animals from the excreta of waterfowl, which
can spread infection. But no such protections are in effect at markets such as
Jiangfeng, which, like the rest of southern China’s booming poultry industry,
lies within the East Asian flyway, one of the world’s most important waterbird
migration routes.
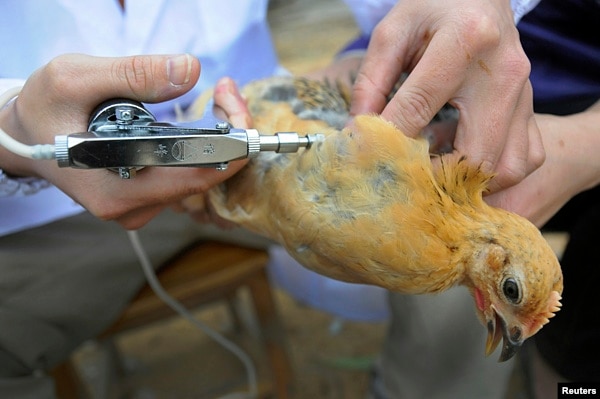
The poultry enclosures are open to the air. Droppings from the birds in
cages as well as the birds flying overhead coat the floor. Stonyfaced women
with shovels push the mess into reeking, shoulder height heaps of wet mush.
Any virus that lurks in those piles can easily spread to the birds and the people
who tend them. Up to 10 percent of poultry workers in Hong Kong, a study has
found, have been exposed to bird flu. A fine dust of desiccated bird waste
permeates the air. It settles on the leaves of the workers’ makeshift vegetable
plots behind the cages and on the window panes of their nearby flats.
These markets and the unique viral ecology they enable are not new, as
Malik Peiris, a virologist at the University of Hong Kong, points out. But “now
the situation is very different,” he said. “This is being done on a much bigger
scale than it was years ago.”
As health conscious consumers in the West cut beef out of their diets and
newly affluent Asians add more meat to theirs, demand for bird flesh has
skyrocketed. Global poultry production has more than quadrupled since 1970. And nowhere has the taste for poultry risen faster than in Asia, where chicken
farming expanded by nearly 4.5 percent a year from 2000 to 2012. China now
consumes more chicken than the United States. Tyson Foods aims to double
production in China. “We just can’t build the houses fast enough,” Donnie
Smith, the company’s chief executive, said to The Wall Street Journal,
referring to poultry production buildings, and “we’re going absolutely as fast
as we know how to go.”
It’s not just the growing scale of the poultry industry in Asia that increases
the probability that new avian influenza viruses will emerge. It’s also the
peculiar nature of the trade. About half of China’s poultry trade traffics in live
birds. That’s because many Chinese consumers, wary of the safety of frozen
meats, prefer to buy their chickens while they’re still clucking. This creates a
wealth of opportunities for new viral strains to spread and adapt to human
bodies. Rather than visiting the sterile frozen food aisles of grocery stores,
shoppers crowd into poultry markets, exposing themselves to live birds and
their viral laden waste. And to serve the markets, more birds travel from farms
into towns and cities, broadcasting viruses along the way.
Most novel strains of avian influenza cannot infect humans. But some can,
including three currently circulating strains: H5N1, a mashup of viruses from
geese and quail; H7N9, an amalgam of viruses from ducks, migratory birds
and chickens; and H10N8, the product of viruses from wild birds, ducks and
chickens. These viruses kill roughly 30 percent to 60 percent of their reported
human victims. None can spread efficiently from one person to another, for
example through sneezes and coughs, yet. But, given the opportunity, they will
continue to evolve. And if they finetune their transmissibility among humans,
the result will almost certainly be the kind of pandemic that epidemiologists
most fear — one that could sicken a billion, kill 165 million and cost the global
economy up to $3 trillion.
A majority of experts predicted, in a 2006 survey, that a pandemic would
occur within two generations. That prediction is based, in part, on the increasing number of novel strains of avian influenza and the accelerating
speed of their emergence. It’s also based on history. The virus that caused the
influenza pandemic of 2009 killed an estimated 200,000 people, hitting young
people in the Americas hardest. It originated in birds. So did the 1918 flu,
which killed 50 million, including an estimated 675,000 Americans.
For years, experts considered the Americas comfortably isolated from the
virulent avian influenza viruses hatched on distant Asian poultry farms and
markets. “Being in North America,” said Carol Cardona, an avian disease
expert at the University of Minnesota, “we weren’t bothered.”
Some of the novel strains of avian influenza emerging from the Asian
poultry trade can be picked up and spread far and wide by migratory birds. But
the migratory routes of these birds don’t cross the oceans. Even as they spread
H5N1 and other pathogens into dozens of countries in Europe, Asia and Africa,
the Americas remained untouched.
That changed in late 2014, when a highly virulent avian influenza from
Asia infiltrated North America. Its prospects here differed from those in Asia.
Relatively few people are regularly exposed to live poultry and their waste. And
farmers protect their domesticated flocks from pathogens by screening and
controlling ventilation in barns and by regularly disinfecting farm equipment.
Remarkably, none of these safeguards arrested the virus’s inexorable
spread. It was as if the virus “knew the weaknesses of each individual farm,”
said Dr. Cardona, “and found that and exploited it.” Infected farms euthanized
entire flocks by smothering them with carbon dioxide or firefighting foam.
From December 2014 to last June, more than 48 million domesticated poultry
in 21 states were slaughtered, the majority in waterfowl rich Minnesota and
Iowa, in what the Department of Agriculture called the worst animal disease
epidemic in United States history. By the time it ended, a 12 foot wide ridge of
bird carcasses from a single farm in Iowa stretched more than six miles.
Nobody knows just how this virus migrated over the oceans protecting the New World. But it’s possible that another consequence of human appetites —
climate change — played a role.
While Asian and European birds don’t migrate into North America, they
can pass on viruses to birds that do. That could happen in a place where
millions of birds from both the Old World and New World are instinctively
drawn every spring: the Arctic lands surrounding the Bering Strait, known as
Beringia.
In the past, New and Old World birds in Beringia visited numerous ponds
spread out across the tundra. But with temperatures in the Arctic rising twice
as fast as anywhere else, conditions are changing rapidly, shifting the
distribution of creatures and their pathogens. Historically segregated species
are coming into novel kinds of contact. As birds are forced to migrate earlier
and farther, feeding at new times and in new places, they overlap with other
bird species in unprecedented ways that pathogens can exploit.
Some already have. In 2012, a parasitic roundworm normally found some
1,000 miles southeast turned up in birds in western Alaska. In 2013, birds in
Alaska suffered their first epidemic of avian cholera, which typically infects
birds in the lower 48 states.
WHILE the precise conditions under which the virulent Asianorigin virus
arrived in North America in 2014 remain murky, what’s known is this:
Migratory birds picked up the virus from a poultry farm in Asia, carrying it
with them into Siberia and Beringia for the breeding season. There, whether it
was because of the new intimacy of the changed landscape, or because of
something about the virus itself, the pathogen spread into other bird species,
including those that would later head into North America, such as gyrfalcons
and northern pintail ducks. By December 2014, they had brought the virus
into British Columbia, Washington and Oregon, infecting wild and
domesticated birds along the way and igniting the epidemic.
If this strain had been one that could infect humans, a deadly and disruptive public health emergency would have ensued. Luckily, it was not.
But there are more where it came from, at the growing interface between
live poultry and humans on the other side of the Pacific. The workers at
Jiangfeng, with their bare hands and tall boots, toil at its border. I watched
them in the crowded enclosures as they lassoed birds around the neck with
long, curved poles, stuffing them into plastic bins and loading them onto
trucks. When a security guard caught me staring, I quickly walked away,
footsteps muted by the membrane of bird waste encasing the soles of my
shoes. Perhaps I could scrounge some bleach solution at my hotel with which
to sterilize them, I thought to myself, although of course the birds whose lives
and peregrinations are shaped by our appetites would not be so circumspect.
As I padded toward the exit, a stream of vehicles crammed with fowl, and
whatever viruses replicated inside their feathery bodies, steadily rumbled out
of the market, bound for points unknown.